Nutrition Considerations for Vegetarians, Part 2
Contributed by Maggie Collins, MPH, RDN, CDCES, DipACLM
A vegetarian diet has been associated with a vast array of health benefits, but what makes it so powerful in preventing, managing, or even reversing chronic diseases is not only the elimination of meat and other animal products, but also the plant-based food choices that are made. In this upcoming webinar we will discuss what are the nutrients of “concern” on a plant-based diet and how to make sure we are not falling short on them to guarantee we are doing the best we can in optimizing our health.
Plant-based diets have gained a lot of attention from science and from the media in the past decades. Seventh-Day Adventists (SDAs) is one of the groups that have been highlighted in scientific articles and magazines like the National Geographic because of the health benefits found in those who follow a vegan or vegetarian diet, including the reduced risk for cardiovascular disease, diabetes, obesity, several types of cancer, and up to 10 extra years of life when compared to the general population [1-4].
As mentioned on the part 1 of this article (See article NUTRITION CONSIDERATIONS FOR VEGETARIANS, Part 1) The Academy of Nutrition and Dietetics (AND) on its position paper on vegetarian diets also supports the health advantages of a vegan or vegetarian diet. However, they emphasize key nutrients that those following a plant-based diet should take into consideration when planning their meals. On part 1 of this article we discussed four of those nutrients: protein, zinc, iron, and calcium. The other four nutrients those following plant-based diets should pay special attention to are: omega-3, vitamin D, iodine, and vitamin B-12. We will examine three aspects of these nutrients:
- What is their function in the body.
- What is their daily recommended intake.
- What foods are rich in these nutrients.
Omega-3
Omega-3 is one of the essential fats associated with a myriad of health benefits, including brain and retina development (critical for fetal development during pregnancy), cognitive function, immune function, nervous system function, cell membrane structure, and anti-inflammatory properties [5]. An adequate amount of omega-3 fatty acids has also been associated with a reduced risk of chronic diseases [6, 7].
The types of Omega-3 fatty acids include α-linolenic acid (ALA), stearidonic acid, eicosapentaenoic acid (EPA), docosapentaenoic acid (DPA), and docosahexaenoic acid (DHA). Some health benefits associated with omega-3s are linked specifically to EPA and DHA (found mainly in fatty fish and microalgae). The most commonly consumed plant source of omega-3, ALA, can be converted in our bodies into EPA and DHA but this process is dependent on other factors, such as dietary choices, genetics, gender (young males convert less efficiently than young females), advancing age, the presence of chronic disease, and smoking [8].
Although there is evidence that vegetarians and vegans have lower blood and tissue levels of EPA and DHA [8, 9] than nonvegetarians, studies indicate that children and adults that follow these eating patterns don’t seem to present signs of clinical deficiencies [2, 8, 9]. Nonetheless, it seems prudent to continue to pursue adequacy of these important nutrients by following three steps:
- A regular intake of ALA-rich plant sources to meet the daily needs.
- Adopting dietary modifications to facilitate the conversion of ALA into EPA and DHA.
- Taking an algae-based EPA and DHA supplement as needed. A supplement of 200-300 mg/day of EPA and DHA is suggested for vegan or vegetarian pregnant and lactating women, the elderly and those with chronic diseases. [8]
Daily Omega-3 Needs
Recommended Dietary Allowances (RDAs) for Omega-3 [10]
| Age | Male | Female | Pregnancy | Lactation |
|---|---|---|---|---|
| Birth to 6 months* | 0.5 g | 0.5 g | ||
| 7 – 12 months* | 0.5 g | 0.5 g | ||
| 1 – 3 years** | 0.7 g | 0.7 g | ||
| 4 – 8 years** | 0.9 g | 0.9 g | ||
| 9 – 13 years** | 1.2 g | 1.0 g | ||
| 14 – 18 years** | 1.6 g | 1.2 g | 1.4 g | 1.3 g |
| 19+ years** | 1.6 g | 1.1 g | 1.4 g | 1.3 g |
* As total omega-3
** As ALA
Omega-3 Content of Selected Plant-Based Foods
| Food Source | Serving | Total Amount of ALA |
|---|---|---|
| Walnuts | ¼ cup | 2.6 g |
| Flaxseed oil | 1 tsp | 2.4 g |
| Flaxseeds, whole | t Tbsp | 2.3 g |
| Chia seeds | 1 Tbsp | 1.7 g |
| Hemp seeds | 2 Tbsp | 1.7 g |
| Canola oil | 1 Tbsp | 1.3 g |
| Tofu, firm | ¼ block | 0.8 g |
| Edamame | 1 cup | 0.6 g |
Source: U.S. Department of Agriculture, Agricultural Research Service. FoodData Central, 2019. fdc.nal.usda.gov.
Suggested Dietary Modifications
- Because omega-3 and omega-6 use the same enzyme in their process of conversion to their respective long-chain fatty acids, one of the steps that help increase EPA and DHA conversion from ALA is to reduce the intake of omega-6 rich foods, especially from oils such as corn oil, safflower oil, soybean oil, sunflower oil, cottonseed oil, and peanut oil.
- Avoid alcohol or caffeine, as they can reduce the body’s ability to convert ALA.
- Avoid trans fats. Thankfully trans fats are currently banned in the U.S., but when traveling to other countries this type of fat is found in hydrogenated and partially-hydrogenated oils, so reading the ingredients in the label will help to identify it.
- A diet that is deficient in protein, vitamins (especially niacin, pyridoxine, and vitamin C) and minerals (especially zinc and magnesium) can also affect this process as it diminishes the activity of conversion enzymes. Thus, is important to ensure the diet is providing sufficient calories to maintain a healthy weight and includes a variety of healthy plant foods, such as fruits, vegetables, whole grains, beans, lentils, peas, nuts and seeds.
- Some experts also suggest doubling the ALA intake based on the RDA, except when taking an algae supplement of EPA and DHA.

Vitamin D
Vitamin D is a fat-soluble vitamin involved in calcium absorption in the gut; bone growth, remodeling, and mineralization; immune function; cell growth modulation; reduction of inflammation; glucose metabolism; and neuromuscular function [13].
Vitamin D can be obtained from four sources:
- Vitamin D production from this source is dependent on several factors, such as the time of the day, latitude, season, air pollution, skin coverage with clothes, age, and skin pigmentation.
- Naturally occurring dietary sources: fatty fish, fish liver oil and mushrooms exposed to UV light have high concentrations of vitamin D; beef liver, egg yolk, regular mushroom, and cheese have a marginal amount.
- Fortified dietary sources: found in milk, some plant-based milk substitutes, some breakfast cereals, some brands of orange juice, yogurt, and other food products. Refer to the label to find the products that are fortified with vitamin D.
- Supplements: vitamin D3 or vitamin D2.
Low vitamin D intake and low laboratory values have been reported on some vegetarians or vegans, the latter especially during winter or spring or among those living in high altitudes[14]. Considering that the highest concentration of vitamin D naturally occurring in foods is found in fatty fish, the use of foods fortified with vitamin D and supplements are commonly recommended to meet the needs of this nutrient among those eating a plant-based diet.
Vitamin D supplementation should be discussed with a healthcare provider, and should be based on the assessment of laboratory values. Other risk factors for vitamin D deficiency to also consider supplementation include obesity, Crohn’s disease, celiac disease, ulcerative colitis, liver disease, kidney disease, breastfed infants, old age, dark skin, wearing covering clothes that prevents the exposure of the skin to sunlight, and irregular sunshine exposure [15-17].
Daily Vitamin D Needs
Recommended Dietary Allowances (RDAs) for Vitamin D [18]
| Age | Male | Female | Pregnancy | Lactation |
|---|---|---|---|---|
| 0 – 12 months | 10 mcg (400 IU) | 10 mcg (400 IU) | ||
| 1 – 13 years | 15 mcg (600 IU) | 15 mcg (600 IU) | ||
| 14 – 18 years | 15 mcg (600 IU) | 15 mcg (600 IU) | 15 mcg (600 IU) | 15 mcg (600 IU) |
| 19 – 50 years | 15 mcg (600 IU) | 15 mcg (600 IU) | 15 mcg (600 IU) | 15 mcg (600 IU) |
| 51 – 70 years | 15 mcg (600 IU) | 15 mcg (600 IU) | ||
| >70 years | 20 mcg (800 IU) | 20 mcg (800 IU) |
Vitamin D Content of Selected Plant-Based Foods
| Food Source | Serving | mcg | IU |
|---|---|---|---|
| Mushrooms, white, raw, sliced, exposed to UV light | ½ cup | 9.2 | 366 |
| Soy, almond, and oat milks, vitamin D fortified, various brands | 1 cup | 2.5 – 3.6 | 100 – 144 |
Source: U.S. Department of Agriculture, Agricultural Research Service. FoodData Central, 2019. fdc.nal.usda.gov.

Iodine
Iodine makes up an important component of the thyroid hormones thyroxine (T4) and triiodothyronine (T3). These hormones are involved in protein synthesis, skeletal and central nervous system development in fetuses and infants, and many metabolic activities [19].
Daily Iodine Needs
Recommended Dietary Allowances (RDAs) for Iodine [19]
| Age | Male | Female | Pregnancy | Lactation |
|---|---|---|---|---|
| 0 – 6 months | 110 mcg | 110 mcg | ||
| 7 – 12 months | 130 mcg | 130 mcg | ||
| 1 – 3 years | 90 mcg | 90 mcg | ||
| 4 – 8 years | 90 mcg | 90 mcg | ||
| 9 – 13 years | 120 mcg | 120 mcg | ||
| 14 – 18 years | 150 mcg | 150 mcg | 220 mcg | 290 mcg |
| 19+ years | 150 mcg | 150 mcg | 220 mcg | 290 mcg |
Iodine can be obtained from three sources:
- Some foods
- Fortified table salt
- Dietary supplement
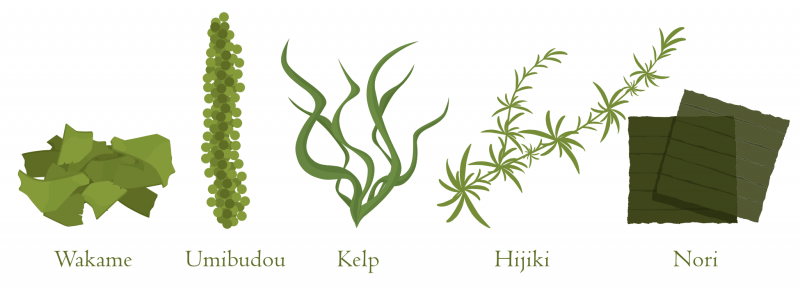
The Iodine content in the soil varies, affecting the content in crops. Seaweed (such as nori, kelp, kombu, and wakame) is one of the best dietary sources of iodine [20]. Other good sources include seafood, milk (not naturally occurring, but present in milk from the iodine used to disinfect the teats of the cows or from iodine containing supplements feds to the cows), and eggs. Iodine is also present in breast milk and infant formulas [19-21].
Vegans and Vegetarians who do not consume iodized salt or seaweed regularly may be at risk of iodine deficiency and should consider taking a supplement. Vegan women of child-bearing age are encouraged to supplement with 150 mcg iodine/day, since the fetus and breast-fed infants rely on maternal iodine for proper thyroid hormones synthesis required for a normal neurodevelopment [22]. A state of iodine deficiency during this stage could lead to permanent mental retardation [23]. It is important to add, however, that the risk for iodine deficiency is not exclusive of this population. According to the American Thyroid Association, many parts of the world do not have enough iodine available through their diet leading to an estimate of about 30% of the world’s population being at risk for iodine deficiency [24].
Iodine Content of Selected Plant-Based Foods
| Food Source | Serving | Iodine Content (mcg) |
|---|---|---|
| Seaweed | 1 g | 16 – 2,984 mcg |
| Kelp | 1 Tbsp | 2,000 mcg |
| Kombu | 1-inch piece | 1,400 mcg |
| Hiziki* | 1 Tbsp | 780 mcg |
| Arame | 1 Tbsp | 730 mcg |
| Nori seaweed, dried | 0.6 oz | 388 mcg |
| Wakame | 1 Tbsp | 80 mcg |
| Iodized salt | ¼ tsp | 71 mcg |
| Lima beans, cooked | 1 cup | 16 mcg |
| Prunes | 5 | 13 mcg |
Source: U.S. Department of Agriculture, Agricultural Research Service. FoodData Central, 2019. fdc.nal.usda.gov.
* There is a warning that this seaweed contains too much arsenic, which can increase the risk of cancer.
Since a significant amount of iodine is stored in the thyroid gland, some experts suggest that the occasional consumption of seaweed would be sufficient to ensure iodine adequacy [26]. However, it is important to consider that some seaweed have extremely high iodine content, which can lead to hyperthyroidism, so it is important to not overdo on this dietary source either.
Vitamin B-12
Vitamin B12 is required for the development, and maintenance of the central nervous system; DNA and red blood cell synthesis. In addition, vitamin B12 functions as a cofactor for enzymes involved in the synthesis of the essential amino acid methionine (required for many processes in the body) and of the short-chain fatty acid propionate (a substance that is thought to reduce the storage of fat in the body, reduce cholesterol levels, and even reduce the risk of cancer) [27, 28].
Vitamin B-12 Daily Needs
Recommended Dietary Allowances (RDAs) for Vitamin B12 [29]
| Age | Male | Female | Pregnancy | Lactation |
|---|---|---|---|---|
| 0 – 6 months* | 0.4 mcg | 0.4 mcg | ||
| 7 – 12 months* | 0.5 mcg | 0.5 mcg | ||
| 1 – 3 years | 0.9 mcg | 0.9 mcg | ||
| 4 – 8 years | 1.2 mcg | 1.2 mcg | ||
| 9 – 13 years | 1.8 mcg | 1.8 mcg | ||
| 14 – 18 years | 2.4 mcg | 2.4 mcg | 2.6 mcg | 2.8 mcg |
| 19+ years | 2.4 mcg | 2.4 mcg | 2.6 mcg | 2.8 mcg |
* Adequate Intake (AI)
Vitamin B12 can be obtained from four sources:
- Naturally present in some foods (meats, dairy, and eggs).
- Fortified into some foods (such as plant-based dairy substitutes, nutritional yeast, and meat analogues).
- Dietary supplements.
- Prescription (usually in more concentrated forms delivered as a shot).
If animal products are completely eliminated from the diet, foods fortified with vitamin B-12 should be consumed on a regular basis. Otherwise, supplementation is indicated.
Because there is no plant-based food with a natural reliable or significant source of vitamin B-12, those who wish to meet some or all of their vitamin B12 needs from fortified foods should refer to the label of the products for their B-12 content.
For those who decide to just monitor their vitamin B12 lab results and start supplementation when they drop, it is important to request additional laboratory tests for a more precise measurement as the typical test ordered to measure serum B12 in the blood may not show signs of deficiency early enough. The additional tests recommended are Methylmalonic Acid (MMA) levels and homocysteine levels[28]. It may not be wise to wait for the B12 levels to drop to a deficient state before considering supplementation as some neurological damage may be irreversible. Talk to your doctor to discuss what supplements are best for you based on your medical condition, blood work and eating habits.
Other groups at risk for vitamin B-12 deficiency include older adults, those suffering from pernicious anemia, those with anthropic gastritis, those with gastrointestinal disorders (such as
Crohn’s disease, celiac disease), individuals with diabetes taking Glucophage (Metformin), and individuals who had gastrointestinal surgery [28, 30].
Summary
The progress of science has revealed the many health benefits of a well-planned plant-based diet, but has also brought to light some nutrients that require special attention. With this information, one may be tempted to think that eating a plant-based diet is complicated, but as we take small steps to implement what we learn, we develop habits that makes the process progressively easier and enjoyable. An annual blood work, or as often as indicated by your healthcare provider, can help direct dietary adjustments and decisions about supplementation.
The responsibilities involved in planning a healthy diet are not excluded from those eating other dietary patterns. Therefore, a plant-based diet should not be perceived as a choice that involves more work but rather as a lifestyle that when followed properly can lead to superior health outcomes as it has been associated with less illnesses and greater longevity, beings endorsed by both biblical and scientific evidence (see article on “Finding True Joy in Eating”).
To keep the body in a healthy condition, in order that all parts of the living machinery may act harmoniously, should be the study of our life. Counsels on Diet and Foods 5.4

References
- Fraser, G.E. and D.J. Shavlik, Ten Years of Life: Is It a Matter of Choice? Archives of Internal Medicine, 2001. 161(13): p. 1645-1652.
- Orlich, M.J., et al., Vegetarian dietary patterns and mortality in Adventist Health Study 2. JAMA internal medicine, 2013. 173(13): p. 1230-1238.
- Tantamango-Bartley, Y., et al., Vegetarian diets and the incidence of cancer in a low-risk population. Cancer Epidemiol Biomarkers Prev, 2013. 22(2): p. 286-94.
- Buettner, D. and S. Skemp, Blue Zones: Lessons From the World’s Longest Lived. Am J Lifestyle Med, 2016. 10(5): p. 318-321.
- Shahidi, F. and P. Ambigaipalan, Omega-3 Polyunsaturated Fatty Acids and Their Health Benefits. Annual Review of Food Science and Technology, 2018. 9(1): p. 345-381.
- Melina, V., W. Craig, and S. Levin, Position of the Academy of Nutrition and Dietetics: Vegetarian Diets. J Acad Nutr Diet, 2016. 116(12): p. 1970-1980.
- Trumbo, P., et al., Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein and amino acids. J Am Diet Assoc, 2002. 102(11): p. 1621-30.
- Saunders, A.V., B.C. Davis, and M.L. Garg, Omega-3 polyunsaturated fatty acids and vegetarian diets. Med J Aust, 2013. 199(S4): p. S22-6.
- Sanders, T.A., DHA status of vegetarians. Prostaglandins Leukot Essent Fatty Acids, 2009. 81(2-3): p. 137-41.
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. 2005, Washington, DC: The National Academies Press. 1358.
- Das, U.N., Essential fatty acids: biochemistry, physiology and pathology. Biotechnol J, 2006. 1(4): p. 420-39.
- Brenda Davis, V.M., Becoming Vegan Express Edition. 2013: Summertown, Tennessee.
- Office of Dietary Supplements. Vitamin D. August 17, 2021; Available from: https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/#en1.
- Mangels, A.R., Bone nutrients for vegetarians. Am J Clin Nutr, 2014. 100 Suppl 1: p. 469s-75s.
- Zemb, P., et al., Vitamin D deficiency and the COVID-19 pandemic. J Glob Antimicrob Resist, 2020. 22: p. 133-134.
- Nair, S., Vitamin d deficiency and liver disease. Gastroenterology & hepatology, 2010. 6(8): p. 491-493.
- Restrepo Valencia, C.A. and J.V. Aguirre Arango, Vitamin D (25(OH)D) in patients with chronic kidney disease stages 2-5. Colombia medica (Cali, Colombia), 2016. 47(3): p. 160-166.
- Institute of Medicine Committee to Review Dietary Reference Intakes for Vitamin, D. and Calcium, The National Academies Collection: Reports funded by National Institutes of Health, in Dietary Reference Intakes for Calcium and Vitamin D, A.C. Ross, et al., Editors. 2011, National Academies Press (US). Copyright © 2011, National Academy of Sciences.: Washington (DC).
- Institute of Medicine Panel on, M., in Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc. 2001, National Academies Press (US). Copyright 2001 by the National Academy of Sciences. All rights reserved.: Washington (DC).
- Zimmermann, M.B., Iodine deficiency. Endocr Rev, 2009. 30(4): p. 376-408.
- Office of Dietary Supplements. Iodine. March 29, 2021; Available from: https://ods.od.nih.gov/factsheets/Iodine-HealthProfessional/#en1.
- Leung, A.M., et al., Iodine status and thyroid function of Boston-area vegetarians and vegans. The Journal of clinical endocrinology and metabolism, 2011. 96(8): p. E1303-E1307.
- World Health Organization. Assessment of iodine deficiency disorders and monitoring their elimination : a guide for programme managers. 2007, World Health Organization: Geneva.
- American Thyroid Association . Iodine Deficiency. Available from: https://www.thyroid.org/iodine-deficiency/.
- Choudhry, H. and M. Nasrullah, Iodine consumption and cognitive performance: Confirmation of adequate consumption. Food Sci Nutr, 2018. 6(6): p. 1341-1351.
- Combet, E., 42 – Iodine Status, Thyroid Function, and Vegetarianism, in Vegetarian and Plant-Based Diets in Health and Disease Prevention, F. Mariotti, Editor. 2017, Academic Press. p. 769-790.
- Hosseini, E., et al., Propionate as a health-promoting microbial metabolite in the human gut. Nutr Rev, 2011. 69(5): p. 245-58.
- Office of Dietary Supplements.. Vitamin B12. April 6, 2021; Available from: https://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/.
- Institute of Medicine Standing Committee on the Scientific Evaluation of Dietary Reference, I., O.B.V. its Panel on Folate, and Choline, The National Academies Collection: Reports funded by National Institutes of Health, in Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B(6), Folate, Vitamin B(12), Pantothenic Acid, Biotin, and Choline. 1998, National Academies Press (US). Copyright © 1998, National Academy of Sciences.: Washington (DC).
- Kim, J., et al., Association between metformin dose and vitamin B12 deficiency in patients with type 2 diabetes. Medicine, 2019. 98(46): p. e17918-e17918.

[…] Vitamin D – According to the most recent meta-analysis on the effects of Vitamin D supplementation on participants with depression, vitamin D supplementation did not show to have a significant impact in reducing depression symptoms [37]. However, the majority of the studies have looked at individuals with low levels of depression and sufficient vitamin D at baseline. On the other hand, another meta-analysis has concluded that a low vitamin D concentration is associated with depression [38]. Therefore, while we wait for the gap in the scientific literature to investigation the impact the effects of vitamin D supplementation on individuals who are both depressed and vitamin D deficient, it certainly makes sense to ensure adequate vitamin D levels are maintained. For information on how much vitamin D we need per day to maintain adequate levels and good sources of vitamin D, refer to the article Nutrition Considerations for Vegetarians, Part 2. […]